Practice Essentials
Superior mesenteric artery (SMA) syndrome is an uncommon but well recognized clinical entity characterized by compression of the third, or transverse, portion of the duodenum between the aorta and the superior mesenteric artery. This results in chronic, intermittent, or acute complete or partial duodenal obstruction. [1, 2] See the image below.
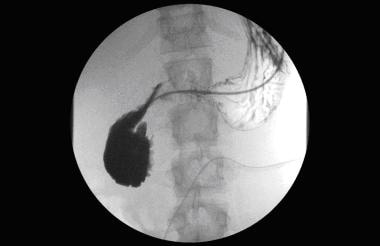 Prompt gastric emptying of residual contrast is present within the stomach into the second portion of the duodenum. Additional contrast was hand injected through the transpyloric feeding tube to further distend the second portion of the duodenum. The second portion of the duodenum is dilated with very slow transit across the spine into the jejunum. This occurred despite difference in position of the patient. The high-grade partial obstruction at the distal second portion of the duodenum is due to superior mesenteric artery (SMA) syndrome.
Prompt gastric emptying of residual contrast is present within the stomach into the second portion of the duodenum. Additional contrast was hand injected through the transpyloric feeding tube to further distend the second portion of the duodenum. The second portion of the duodenum is dilated with very slow transit across the spine into the jejunum. This occurred despite difference in position of the patient. The high-grade partial obstruction at the distal second portion of the duodenum is due to superior mesenteric artery (SMA) syndrome.
Superior mesenteric artery syndrome was first described in 1861 by Von Rokitansky, who proposed that its cause was obstruction of the third part of the duodenum as a result of arteriomesenteric compression. Some studies report the incidence of superior mesenteric artery syndrome to be 0.1-0.3%. [3] Approximately 0.013-0.78% of barium upper GI studies evaluating for superior mesenteric artery syndrome support the diagnosis. [4, 5]
Despite the fact that about 400 cases are described in the English language literature, many have doubted the existence of SMA syndrome as a real entity; indeed, some investigators have suggested that superior mesenteric artery syndrome is overdiagnosed because it is confused with other causes of megaduodenum. Nonetheless, the entity (also called cast syndrome) is a well-known complication of scoliosis surgery, anorexia, and trauma. It often poses a diagnostic dilemma; its diagnosis is frequently one of exclusion.
Signs and symptoms
Patients often present with chronic upper abdominal symptoms such as abdominal pain, nausea, eructation, voluminous vomiting (bilious or partially digested food), postprandial discomfort, early satiety, and sometimes subacute small bowel obstruction.
See Presentation for more detail.
Diagnosis
The diagnosis of SMA syndrome is difficult. Confirmation usually requires radiographic studies, such as an upper GI series, hypotonic duodenography, and CT scanning.
See Workup for more detail.
Management
Reversing or removing the precipitating factor is usually successful in a patient with acute SMA syndrome. Conservative initial treatment is recommended for all patients; this includes adequate nutrition, nasogastric decompression, and proper positioning of the patient after eating.
Surgical intervention is indicated when conservative measures are ineffective, particularly in patients with a long history of progressive weight loss, pronounced duodenal dilatation with stasis, and complicating peptic ulcer disease.
See Treatment and Medication for more detail.
Pathophysiology
The superior mesenteric artery usually forms an angle of approximately 45° (range, 38-56°) with the abdominal aorta, and the third part of the duodenum crosses caudal to the origin of the superior mesenteric artery, coursing between the superior mesenteric artery and aorta. Any factor that sharply narrows the aortomesenteric angle to approximately 6-25° can cause entrapment and compression of the third part of the duodenum as it passes between the superior mesenteric artery and aorta, resulting in SMA syndrome.
In addition, the aortomesenteric distance in superior mesenteric artery syndrome is decreased to 2-8 mm (normal is 10-20 mm). Alternatively, other causes implicated in superior mesenteric artery syndrome include high insertion of the duodenum at the ligament of Treitz, a low origin of the superior mesenteric artery, and compression of the duodenum due to peritoneal adhesions. [6, 7]
Etiology
Important etiologic factors that may precipitate narrowing of the aortomesenteric angle and recurrent mechanical obstruction include the following:
-
Constitutional factors
Thin body build
Exaggerated lumbar lordosis
Visceroptosis and abdominal wall laxity
Depletion of the mesenteric fat caused by rapid severe weight loss due to catabolic states such as cancer, surgery, burns, trauma, or psychiatric problems
-
Severe injuries, such as head trauma, leading to prolonged bedrest
-
Dietary disorders
Malabsorption
-
Spinal disease, deformity, or trauma (use of body cast in the surgical treatment of scoliosis or vertebral fractures): Superior mesenteric artery syndrome cases after corrective spine surgery are due to the result of spinal elongation, which decreases the superior mesenteric/aortic angle. Postoperative weight loss is an important factor for development of superior mesenteric artery syndrome. Although use of Harrington rods for corrective surgery commonly used in the 1950s and 1960s was an important contributory factor for development of superior mesenteric artery syndrome, newer derotation/translation corrective techniques can also rarely be associated with this disease entity. [9]
-
Rapid linear growth without compensatory weight gain, particularly in adolescents: Adolescents with low body mass index (< 18 kg/m2) may be at higher risk for developing superior mesenteric artery syndrome after spinal fusion for scoliosis than patients with a higher body mass index. [10]
-
Anatomic anomalies (rare)
Abnormally high and fixed position of the ligament of Treitz with an upward displacement of the duodenum
Unusually low origin of the superior mesenteric artery
-
Unusual causes
Epidemiology
United States statistics
The precise incidence of this entity is unknown. In a review of the literature, approximately 0.013-0.78% of the findings from upper GI tract barium studies support a diagnosis of superior mesenteric artery syndrome.
Race-, sex-, and age-related demographics
No racial differences have been identified.
More females are affected by SMA syndrome. In one large series of 75 patients with superior mesenteric artery syndrome, two thirds of the cases involved women, with an average age of 41 years; one third of cases involved men, with an average age of 38 years.
SMA syndrome usually occurs in older children and adolescents. In one report, 75% of the cases occurred in patients aged 10-30 years.
Prognosis
The outcome is excellent if the entity is diagnosed in a timely fashion and if the patient receives appropriate therapy. In the past, deaths due to progressive dehydration, hypokalemia, and oliguria have been reported; most of these occurred in patients in whom the diagnosis was delayed or missed.
Morbidity/mortality
Delay in the diagnosis of SMA syndrome can result in malnutrition, dehydration, electrolyte abnormalities, gastric pneumatosis and portal venous gas, formation of an obstructing duodenal bezoar, hypovolemia secondary to massive GI hemorrhage, and even death secondary to gastric perforation. [2, 14, 15, 16]
Complications
Complications include the following:
-
Electrolyte imbalance (eg, hypokalemia, hypochloremia, metabolic alkalosis)
-
Dehydration
-
Malnutrition
-
Oliguria
-
Hypotension
-
Peptic ulcer disease
-
Aspiration pneumonia
The most frequent complication is gastrointestinal mucosal injury, and the incidence has been reported as 25-59% in patients with SMA syndrome. [17]
-
Prompt gastric emptying of residual contrast is present within the stomach into the second portion of the duodenum. Additional contrast was hand injected through the transpyloric feeding tube to further distend the second portion of the duodenum. The second portion of the duodenum is dilated with very slow transit across the spine into the jejunum. This occurred despite difference in position of the patient. The high-grade partial obstruction at the distal second portion of the duodenum is due to superior mesenteric artery (SMA) syndrome.