Practice Essentials
Sinonasal malignant neoplasms are rare tumors that constitute about 3% of tumors in the upper respiratory tract. Only a fraction arises at the nasal cavity. [1] Imaging is essential to staging nasal cavity tumors locally and ruling out the presence of metastases. Computer tomography (CT) scanning and magnetic resonance imaging (MRI) have replaced plain radiographs in workup because of the fine anatomic detail provided by these imaging modalities. Biopsy of the lesion is commonly performed using a rods lens endoscope in the office under topical or local anesthesia. Surgery is the mainstay of treatment for most sinonasal tumors.
Due to the contiguity of the nasal cavities with the paranasal sinuses, identifying the specific site of origin of large sinonasal tumors is often difficult. Hence, malignant tumors of the nasal cavities are often grouped with those of the paranasal sinuses. Their proximity to vital structures such as the brain, optic nerves, and internal carotid artery pose significant challenges for their treatment and may be the source of significant morbidity to the patients. Malignant tumors of the sinonasal tract are derived from diverse histologic elements within the nasal cavity. They include those listed below. [2]
Epithelial tumors
These include the following:
-
Transitional cell carcinoma
-
Adenoid cystic carcinoma
-
Olfactory neuroblastoma
-
Undifferentiated carcinoma
-
Nuclear protein in testis
-
SWItch/Sucrose Non-Fermentable (SWI/SNF) complex–deficient sinonasal carcinoma\
-
Sinonasal lymphoepithelial carcinoma
-
Teratocarcinosarcoma
-
Human papillomavirus (HPV)–associated multiphenotypic sinonasal carcinomas
-
Intestinal-type sinonasal adenocarcinoma
-
Non-intestinal–type sinonasal adenocarcinoma
Nonepithelial tumors
These include the following:
-
Soft-tissue sarcoma
-
Leiomyosarcoma
-
Myxosarcoma
-
Connective tissue sarcoma
-
Synovial sarcoma
Mesenchymal tumors
These include the following:
-
Sinonasal glomangiopericytoma
-
Biphenotypic sinonasal sarcoma
-
Chordoma
Lymphoreticular tumors
These include the following:
-
Lymphoma
-
Plasmacytoma
-
Metastatic carcinoma
Other tumors
These include the following:
-
Olfactory neuroblastoma
Emerging tumors
Released in 2022, the fifth edition of the WHO (World Health Organization) Classification of Head and Neck Tumours discussed emerging sinonasal tumors, including the following [2] :
-
IDH2-mutated sinonasal carcinoma
-
DEK-AFF2 carcinoma
Workup
Imaging is essential to staging the tumor locally and ruling out the presence of metastases. CT scanning and MRI have replaced plain radiographs because of the fine anatomic detail provided by these imaging modalities. CT scanning is superior for the evaluation of the bony architecture of the sinonasal tract and skull base. MRI is the best modality for defining soft tissue detail.
Biopsy of the lesion is commonly performed using a rods lens endoscope in the office under topical or local anesthesia. Alternatively, the sampling can be performed in the more controlled environment of an operating room when a deep biopsy is required of if profuse bleeding is anticipated.
Management
Surgery is the mainstay of treatment for most sinonasal tumors. Radiation as the sole modality of treatment is recommended for unresectable cases, poor surgical candidates, or lymphoreticular tumors. Combination therapy of surgery and adjuvant radiotherapy with or without chemotherapy is given in situations with an advanced tumor (T3 and T4), positive surgical margins, perineural spread, perivascular invasion, cervical lymphatic metastasis, and recurrent tumors. Chemotherapy may also have a palliative role for cytoreduction.
Epidemiology
Frequency
The annual incidence of nasal tumors in the United States is estimated to be less than 1 in 100,000 people per year. These tumors occur most commonly in whites, and the incidence in males is twice that of females. [3] Epithelial tumors most commonly present in the fifth and sixth decades of age.
Although tumors of the nasal cavities are equally divided between benign and malignant types, most tumors of the paranasal sinuses are malignant. Approximately 55% of sinonasal tumors originate from the maxillary sinuses, 35% from the nasal cavities, 9% from the ethmoid sinuses, and the remainder from the frontal and sphenoid sinuses. Squamous cell carcinoma is the most common malignant histologic type (approximately 70-80%) followed by adenoid cystic carcinoma and adenocarcinoma (approximately 10% each). [4]
A study by Gerth et al reported the overall incidence of malignant pediatric sinonasal tumors in the United States to be 0.052 per 100,000. The study, which utilized the Surveillance, Epidemiology, and End Results (SEER) database, found that rhabdomyosarcoma was the most frequently occurring malignancy among patients below age 20 years. [5]
Etiology
Exposures to industrial fumes, wood dust, nickel refining, and leather tanning have all been implicated in the carcinogenesis of various types of sinonasal malignant tumors. In particular, wood dust and leather tanning exposures are well associated with increased risk for adenocarcinoma. [6] Other etiologic agents have been reported including mineral oils, chromium and chromium compounds, isopropyl oils, lacquer paint, soldering and welding, and radium dial painting. Tobacco smoking is not considered to be a significant etiologic factor; however, recent studies demonstrated a higher incidence of nasal cancers in cigarette smokers. [3, 7]
Presentation
Tumors of the sinonasal tract commonly present with symptoms that are identical to those caused by inflammatory sinus disease, such as nasal obstruction, nasal discharge, epistaxis, headache, facial pain, and nasal discharge. Tumors of nasal cavities, however, tend to be diagnosed earlier than those of the paranasal sinuses because of the earlier presentation of obstructive symptoms and epistaxis.
To further complicate this issue, 9-12% of patients are frequently asymptomatic. [8] These factors contribute to a delay in diagnoses, and, hence, an advanced stage of disease at the time of diagnosis. Patients with unilateral sinonasal symptoms or those that are associated with unilateral facial swelling, diplopia or blurred vision, unilateral proptosis, and cranial neuropathies should raise a high index of suspicion for sinonasal cancer and warrant urgent evaluation.
Regional and distant metastases are infrequent even in the presence of advanced stage tumors. The incidence of cervical metastases on initial presentation varies from 1-26%, with most large series reporting less than 10%. Distant metastasis on initial presentation is even less common, with most series presenting an incidence of less than 7%. [1] The presence of regional or distant metastases is a poor prognostic sign.
A thorough head and neck examination, cranial nerve assessment, and a nasal endoscopy should be performed in all patients. Physical examination may reveal proptosis, extraocular muscle impairment, mass effect of the cheek, gingival or gingivobuccal sulcus, (eg, ill-fitting dentures) and loose dentition. Numbness or hyperesthesia of the infraorbital (V2) branch of the maxillary nerve strongly suggests malignant invasion (as in the images below).
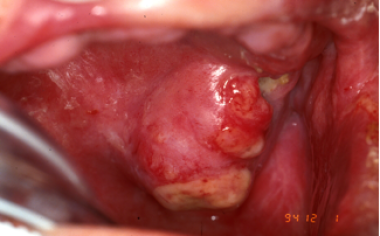 A nasal cavity tumor has eroded through the hard palate and is causing difficulty with fitting a denture.
A nasal cavity tumor has eroded through the hard palate and is causing difficulty with fitting a denture.
Relevant Anatomy
By examining the close relationships of the nasal cavities to the oral cavity, paranasal sinuses, orbit, nasopharynx, pterygomaxillary fissure and pterygopalatine fossa, infratemporal fossa, skull base, and intracranial fossa, one can better understand the myriad signs and symptoms caused by sinonasal tumors.
Local tumor invasion can breach the boundaries of the nasal cavity invading and destroying structures and/or following preformed pathways. The paired nasal cavities are separated by the nasal septum. Their lateral walls comprise the medial wall of the maxillary sinus and the inferior, middle, and superior turbinates. Lateral extension of tumor can infiltrate the maxillary sinus, ethmoid air cells, or even the orbit (through the lamina papyracea). Eventually, orbital involvement manifests as ocular pain, fullness of the eyelid, unilateral epiphora, diplopia, extraocular muscle limitation/diplopia, or proptosis. The floor of the nasal cavity corresponds to the hard palate of the oral cavity; thus, caudal extension of the tumor can present as palatal fullness, pain, and ulceration.
The roof of the nasal cavities is formed by the cribriform plate, which separates the dura of the anterior cranial fossa from the nasal cavity. The cribriform plate, as implied by its name, has multiple openings to accommodate the passage of olfactory filaments. Tumor can spread to the anterior cranial fossa using these openings or by perineural spread. Violation of this barrier during surgery is likely to produce a cerebrospinal fluid (CSF) leak, increasing the risk for meningitis and intracranial abscess. The nasal cavities open externally via the nares and communicate posteriorly with the nasopharynx via the choanae. The eustachian tubes open into the nasopharynx just behind the infero-lateral aspect of the choanae. Tumor extension into the nasopharynx may cause eustachian tube obstruction and secondary serous otitis media that manifests as hearing loss.
Except in the nasal vestibule, the nasal cavity is lined with pseudostratified columnar ciliated epithelium. The nasal vestibule, which corresponds to the ala of the nose, is lined with squamous epithelium containing vibrissae and sweat and sebaceous glands. A small part of the superior portion of the nasal cavity (bound by the superior turbinate laterally and the nasal septum medially) is lined by olfactory epithelium.
The pterygopalatine and infratemporal fossae are important anatomical considerations, as they are densely populated by the mastication muscles, various sensory and motor nerves, and by the blood vessels that supply the nasal cavity, oral cavity, maxillary teeth, pharynx, and ICAs. Tumor extension into these areas can cause a myriad of symptoms, such as the following:
-
Trismus (involvement of the pterygoid muscles or motor branches of the mandibular division of the trigeminal nerve)
-
Facial hypesthesia (involvement of the infraorbital nerve or other sensory branches from the maxillary and mandibular divisions of the trigeminal nerve)
-
Pain in the maxillary dentition (involvement of the anterior, middle, or posterior superior alveolar nerve branches of the maxillary division of the trigeminal nerve)
-
Severe epistaxis (involvement of the terminal branches of the internal maxillary artery)
The pterygopalatine and infratemporal fossae are also potential routes for intracranial tumor spread, via direct extension or hematogenous spread.
Prognosis
A retrospective study by Stepan et al of adult patients with sinonasal rhabdomyosarcoma found a 5-year overall survival rate of 28.4%, with better survival found in patients 35 years or younger at diagnosis (31.9% vs 24.4% for patients over age 35 years). The investigators noted that the 5-year overall survival rate between alveolar and embryonal subtypes (30.5% vs 41.6%, respectively) did not differ by a statistically significant amount but that patients with metastatic disease had worse 5-year overall survival compared with those without (14.7% vs 33.9%, respectively). [9]
-
A nasal cavity tumor has eroded through the hard palate and is causing difficulty with fitting a denture.
-
A nasal tumor that has eroded through the nasal bone and causing deformity of the nasal bridge.
-
Coronal CT scan of the paranasal sinuses illustrating a tumor in the left anterior nasal cavity eroding through the medial orbital wall into the left eye.
-
Coronal MRI T1 with contrast showing an esthesioneuroblastoma of the right nasal cavity eroding the skull base and invading the brain. The maxillary sinus is filled with edematous mucosa.
-
Axial MRI T1 with contrast of the same patient in Image 4 showing mucus in the right sphenoid sinus due to obstruction of the tumor.
-
Axial MRI T1 with contrast showing tumor in the left maxillary sinus with perineural spread in to the left vidian canal.
-
In lateral rhinotomy, a straight incision is made at the naso-maxillary junction followed by a curvilinear incision around the nasal ala.
-
A Weber-Ferguson incision is usually indicated for a total maxillectomy.
-
A cranial base resection with a view of the anterior skull base and nasal cavity from the top.











